The Chronic Phase: Field Trip
The Social Worker at Primary Children’s Hospital told us that writing in a journal can be therapeutic. Even more, perhaps sharing our journey these past few weeks may help other families with children who suffer from this rare, devastating syndrome (F.I.R.E.S. = Febrile Infection-Related Epileptic Syndrome) or other chronic conditions.
Rehab Team, Day #16 (Saturday, September 23rd)
86 days since onset.
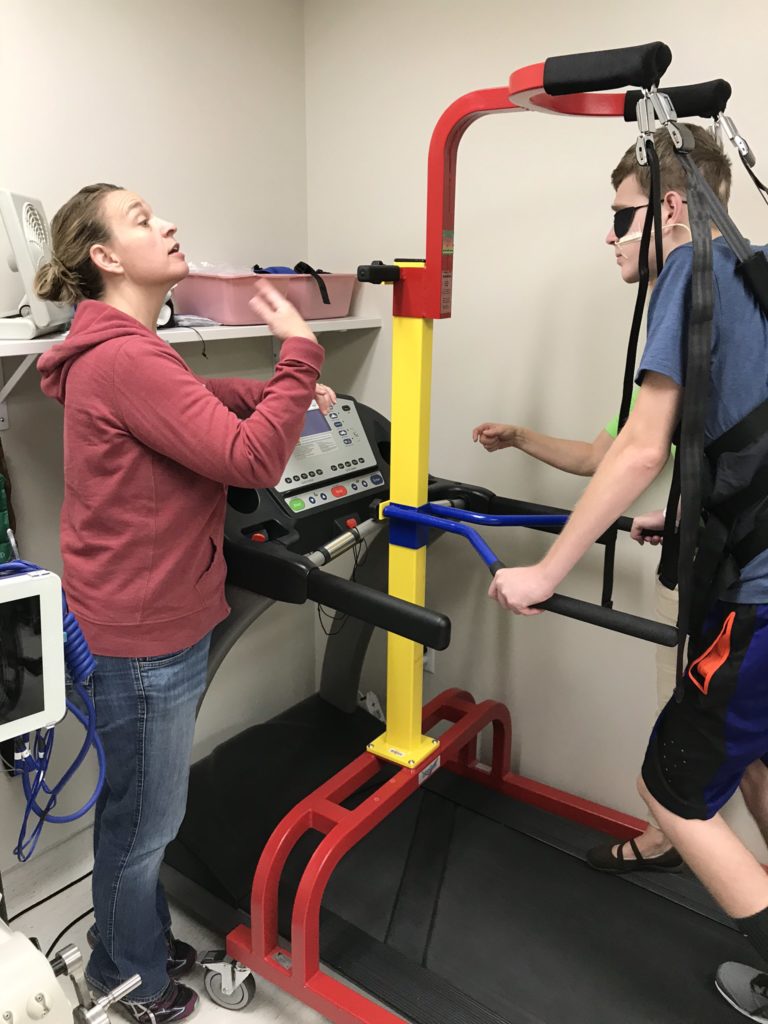
1:30 PM: The morning therapy sessions were the usual dressing, walking, and strengthening activities, but the afternoon physical therapy session involved car transfer training, which was a pre-requisite to leaving the hospital this weekend for a few hours on our Ride Pass. We pulled the car up to the front of the hospital and practiced with the physical therapist. The wind was whipping around and the temperature was chilly as a storm was approaching, but Drew did very well with the car transfer. The nurse also explained to us that as part of the Ride Pass, the doctors and treatment team set 3 goals for us to work on when we leave the hospital. The Ride Pass also allows us to see what gaps remain for Drew to return to home (or other community settings safely.)
4:00 PM: “You know, the ride pass is valid for both Saturday and Sunday,” the nurse explained. “So long as you finish your therapy sessions, which you already have..”
”Really?” Dawn asked. “Maybe we can go for a ride… get out of the hospital for a few minutes.”
”It’s raining,” I said. “And we only have about an hour before his next medicine is due.”
”So what?” Dawn said. “Do you want to go for a ride, Drew?”
”Sure,” he said.
”OK, then, I’ll go pull the car up to the front of the hospital,” I said.
6:00 PM: We drove around the University of Utah campus, up to the front of Hogle Zoo, and then up to Red Butte Gardens, but it was raining pretty hard so we really couldn’t get out of the car. Drew tolerated the car ride without problems and it was good practice.
Rehab Team, Day #17 (Sunday, September 24th)
87 days since onset.
11:15 AM: Drew went to church with Dawn and Erin at the hospital this morning, and still struggled to understand everything said by the speaker. He will make comments out loud, and not in a quiet voice, and today he was quite noticeable.
“I’m broken. I’m broken. I’m broken.” Drew kept repeating this phrase during the closing prayer, but it was so close to being over, they just tried to hush him until the prayer finished.
”What’s the matter, Drew?” His sister asked as the congregation started leaving the chapel.
”The man told me I’m broken,” Drew explained.
”No, he didn’t say that,” his sister said.
”Yes, he did,” Drew said.
”Drew, he didn’t say that, and you’re not broken,” his mother added.
”I’m broken. I’m broken,” Drew continued. “Can I rip this hymn book?” Drew picked up the hymn book from the seat beside his wheelchair.
”No, you can’t rip the hymn book,” his mother said and she carefully took the book from him and returned it to the seat.
For another 45 minutes, he continued to angrily repeat, “I’m broken” before they were able to get him to calm down and focus on something else.
2:45 PM: “How fast is Mom going?” Drew asked me. We were sitting in the middle row of our SUV together. Per the doctors orders, one of us had to sit next to Drew to make sure he had no seizures, stayed upright, and tolerated the drive well.
”Looks like she is going about 70, Drew,” I told him.
”70?” he replied. “Go faster, Mom.”
”I can’t, Drew, it’s raining and the other cars are going slow.”
”I like to drive fast,” Drew whispered to me.
”Not sure I wanted to hear that,” I whispered back.
”Go fast, Mom.”
”I’ll go as fast as I can, Drew,” she said, “but I am more concerned about getting to Grandma’s safely than getting there fast.”
5:30 PM: Drew did fairly well at Grandma’s, but he definitely had trouble navigating stairs, and the more tired he got, the more impulsive and loud he became. Several times, he would try to stand up on his own without warning, and since there were no seatbelts in Grandma’s chairs, we had to be ready to stop or catch him.
He remembered the older cousins fairly well, but it took him several tries to get the younger cousins’ names. Towards the end of the visit it was obvious that he was becoming extremely tired, and as we were preparing to leave, Drew thought it would be funny to drop the F-bomb as he walked toward the door.
”Drew Carter Olsen!” Grandma said.
”I’m just kidding, Grandma,” Drew chuckled.
”That kind of language is NOT funny,” Grandma said with her hands on her hips, “and you don’t talk like that in MY house.”
”OK,” Drew said.
As we were walking down the four stairs into the garage, Drew didn’t even look down, but barreled down them while leaning heavily on my shoulders. I tried to cue him and kept him from falling, but he still rolled his ankle on the last stair.
”Ow, that hurt,” he said. He limped for a few steps, but seemed to be walking fine by the time we got to our car in the driveway. The return to the hospital was uneventful as Drew talked about how much he liked driving fast on the freeway.
Rehab Team, Day #18 (Monday, September 25th)
88 days since onset.
9:30 AM: Pretty good night. Only woke up briefly about 1:00 and pulled on his pulse oximeter and then again at 6:00 when they had to empty his bladder, but both times he went right back to sleep. Drew still gets a little groggy for his morning therapy sessions due to one of his seizure medicines that makes him sleepy, but not as bad as when he was getting the Trazadone. Drank most of his smoothie for breakfast, however, we are grateful that the doctors plan to start weaning him from the Ketogenic diet and will bump his ratio down to 3 fats for every 1 carb and protein combined. The doctors were telling us that even with the extreme ratio of 4.5 to 1, Drew was barely in ketosis so the diet may not have been truly contributing to his seizure control anyway, and with his slow-healing tracheostomy hole and bed sore, we are hoping the increased protein will help them to heal more quickly.
8:30 PM: “I hate your beard,” Drew said. Two of his uncles and two of his cousins had come to visit.
”Why do you hate my beard?” His uncle asked.
”Because, I dont’ like beards,” Drew said. “Have you always had a beard?”
”Drew, don’t you remember? I have had a beard for years,” his uncle said.
”Well, I don’t like it. I think you should leave,” Drew said as he pointed at the door.
”What?” His uncle asked as he looked to us unsure what he should do.
Before we could answer, Drew said, “Just kidding. You can stay, but I still don’t like your beard.”
We tried not to mention beards the rest of the visit.
Rehab Team, Day #19 (Tuesday, September 26th)
89 days since onset.
9:15 AM: Super sleepy this morning even though he slept almost the entire night. He got his medicines at 8:00 AM, and he started falling back to sleep by 8:30 AM. He pretty much slept through OT and they had to reschedule PT because he couldn’t wake up. The nurses didn’t give him any sleep medicines the last few nights, so they are checking again to see if he has a urinary tract infection from all the straight catheters.
10:30 AM: We asked to meet with the dietician about his food. So far, they have brought him the exact same food as when he was on the extreme Ketogenic diet ratio but just a bigger serving without adding any more protein. Last night, he had an egg white and cheese omelet and they doubled the amount of salsa — we were upset because salsa is a condiment!! Then this morning, they doubled the amount of strawberries in his smoothie. He wouldn’t touch the smoothie and we picked some of the strawberries out, but he fell asleep while eating. The doctors and nurses agreed that the diet needs to have more protein, and we asked the dietician to please give him more variety. Really — who eats salsa without chips or something else? That’s not going to help his wounds heal!!
4:30 PM: We just met with the Social Worker who reviewed today’s IDT Meeting discussion and plan for Drew. Short answer is that we will start getting things ready for Drew to discharge from the hospital on either Friday, October 13th or Saturday, October 14th. He will be on a normal diet for his last week in the hospital and they can work with him on swallowing his pills so that hopefully he won’t need the feeding tube at home. The week before he leaves the social worker will also help us order a wheelchair and walker and any other equipment he will need for home, and then she will also help us set up some home or outpatient therapy for continued rehab.
Rehab Team Day #20 (Wednesday, September 27th)
90 days since onset.
4:00 PM: The Rehab doctors came and talked to us about Drew’s sleepiness. His urinary labs came back negative for any infection, and it would simply appear to be that Drew’s seizure medicines are having a greater impact on his alertness. The doctors agreed that they need to start decreasing his seizure medicines so that he can be more awake, but they can only do one at a time and go slow to keep his seizures from returning. Further, the Ketogenic diet is considered to be one of the seizure medicines, but the chances that he is still in ketosis are slim, so they plan to accelerate weaning off of the diet. Tomorrow they will decrease his ratio to 2 fats for every 1 carb and protein, and then starting on Monday he will be on a normal diet.
7:00 PM: ”Why do you have to time how long I eat?” Drew asked.
”Because you take too long,” Dawn tried to explain. “You can’t take 90 minutes to eat your meals.”
”Why does it matter?” Drew asked.
”Because they won’t take out your feeding tube,” Dawn said as she pointed to his face. “Don’t you want your feeding tube out?”
”Of course,” Drew said, “But I don’t seen why it matters how long it takes to eat?”
We are working with Drew to speed up his eating. Every little distraction side rails his focus and he has not regained any automatic behaviors so that he can keep eating while he watches TV or talks. He will take little bites and chew them for several minutes before swallowing, so it just adds up to over an hour to eat a meal. Again, we sure hope he continues to improve and get better.
8:30 PM: “Dad, can you hand me a towel?” Drew asked me.
”Here, use this one.” I handed him the end of the bath blanket hanging from the back of his wheelchair that he had used on his way back from his evening shower. Drew had finished dressing, brushing his teeth, and washing his face.
”Dad, this towel is wet.”
I felt the blanket. “No, Drew, it’s dry.”
”Dad, it’s wet.”
I felt the blanket again, and then I felt his hands. “No, Drew, your hands are wet, not the towel.”
”What?” He asked.
”Your hands are wet. Dry them off on the towel.”
He tried to dry his hands, but then he persisted, “Dad, I need a dry towel.”
His sister then walked over and felt his hands. “Drew, your hands are dry now, but they are ice cold. Let’s warm them up in this blanket.”
She worked for a few minutes until he finally realized what he was feeling and his hands started to warm up.
Rehab Team, Day #21 (Thursday, September 28th)
91 days since onset.
8:15 AM: “Drew, for breakfast they brought you scrambled eggs, a cup of raspberries, and some cream,” I said as I situated his breakfast tray on the table in front of him. Drew was sitting in his wheelchair next to the bed.
”OK,” Drew said.
”Do you want me to put a little raspberry juice in the cream?” I asked.
”Dad, what are you doing? Don’t ruin my milk.”
Drew grabbed the cup of raspberries from me and poured them on his eggs.
“Drew, that is gross.”
”No, Dad, my milk is gross now.”
He mixed them around and started eating them.
Several minutes later, a doctor stopped in to see Drew and he asked Drew what he was eating. Drew said, “scrambled eggs and salsa.”
When the occupational therapist arrived for his OT treatment, Drew was still eating and she asked him, “why are your eggs red?”
Drew answered, “it’s scrambled eggs and salsa.”
I explained that they were raspberries, but to Drew, he finished the plate believing it was salsa that he mixed into his eggs and he couldn’t really tell the difference.
Rehab Team, Day #22 (Friday, September 29th)
92 days since onset. — THREE MONTHS since being admitted to the hospital.
Today was a day of reflection and remembrance for me. Dawn spent the day at the hospital with Drew and said he did well with most of his therapies while I spent the day at home fixing our daughter’s car and installing grab bars for Drew to come home. In the evening, the whole family sat in Drew’s room as his brother and sisters all came to the hospital. We had the BYU-Utah State streaming on Alex’s computer, which served to be a major distraction so that Drew ended up taking 2 hours to eat his dinner (steak and salad).
Although Drew has made a lot progress from the brink of death, the 3-month anniversary of the onset of his illness combined with the prospect of leaving the hospital within the next two weeks has brought more into focus the extent of Drew’s continued impairments and how much our lives will be different now.
I slept poorly the last couple of nights as I keep thinking back to the week before he came to the hospital. He had been running a fever for a few days with some malaise, but really no warning signs of what lie ahead. He talked to me about his workout routine, reviewed his schedule at work for the week, and asked about hanging out with his friends while we sat and ate dinner three nights before he went unconscious. Now we have to help him eat, get dressed, and shower. He has trouble remembering things and struggles at times to find words. His eyes don’t work together and he has to wear an eyepatch. At this point, he also has a hole in his throat and a wound on his tailbone that have yet to heal. His body is weak and his balance is horrible, and to make matters worse, he does not realize his balance is bad and has to be supervised at all times.
In the back of our minds, we were hoping that Drew would be able to rehab back to normal before he left the hospital, with visions of him walking out the front doors of the hospital with his arms raised in victory. However, that seems more fantasy than reality at this point and will likely not be achievable by the time he leaves the hospital in a couple of weeks.
Next summer we were hoping for a family trip to Hawaii to celebrate Drew’s high school graduation and his older sister’s graduation from college, but now the thought of any future family vacations seem as insurmountable as Mount Everest. Even just a trip to the grocery store now appears extremely difficult and frustrating, and will require coordination of efforts and juggling of schedules.
Life will not be the same, and certainly our family is no different from others who face illness or other challenges, but we have to just keep moving forward, grateful in the fact that our family is still whole despite what has been lost, working together to overcome what still lies ahead.

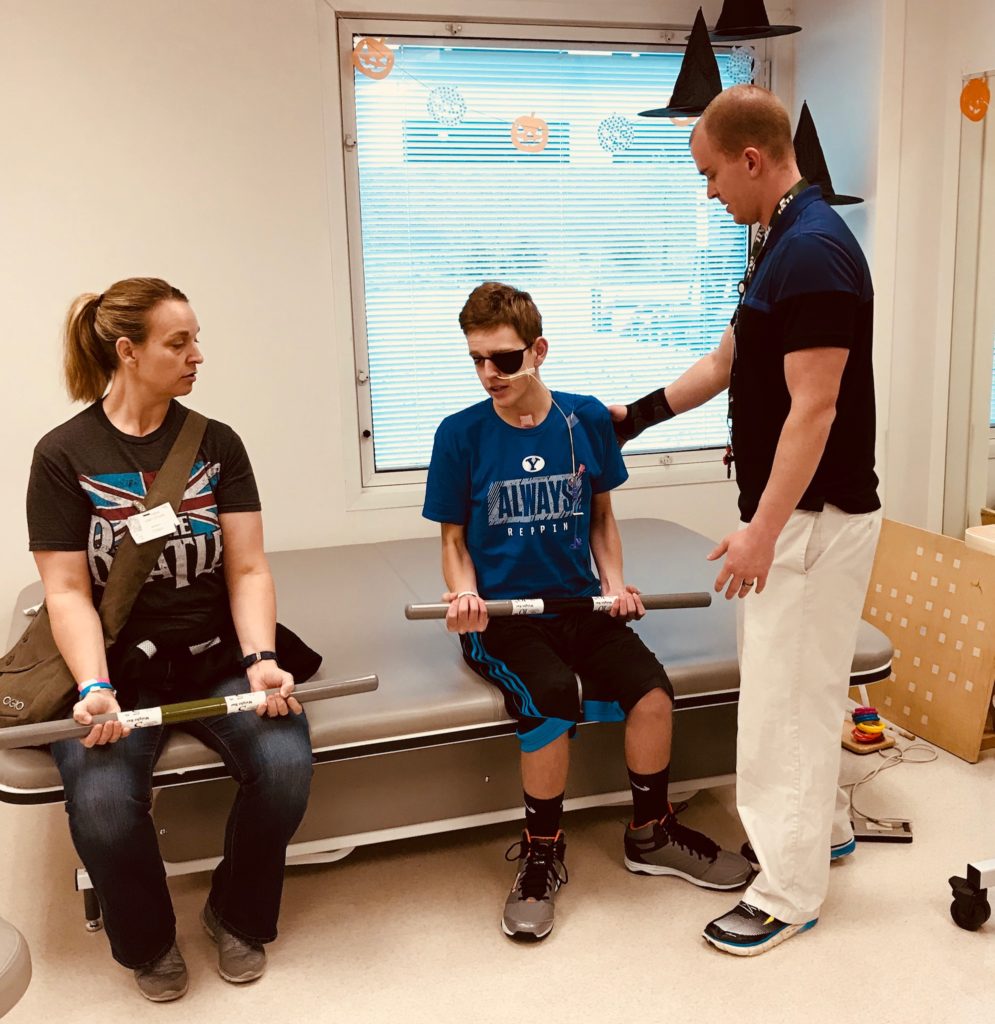
Shooting some hoops in physical therapy. The PT sits behind him to guard him from falling as he works on his balance.
© Copyright 2017 Jeff, All rights Reserved. Written For: Jeffrey Olsen



May the Lord and his angels sustain your family; heal minds, bodies and hearts and give you each hope, energy and patience as you take it one day at a time. Please know Drew and your family are continually in our prayers and hearts. We are amazed at your faith, courage and dedication. Thank you for the continued updates as we cheer your family and Drew on. Love, Camille
Drew, I can’t stand beards, either. 😉 I’m glad you’re making so much progress. Keep it up.
Drew’s progress is amazing although slow. His attitude and determination will help him heal. With God’s love, it will get better for this sweet young man.
Sending continued prayers to all..
One teeny tip that we loved for the grocery, once you are home. Smith’s by us has Clicklist, even Drew could go for the ride to pick up everything. You don’t even get out of the car. It saved my sanity so much. Also have drive through RX. I am sure you guys will find a way to make it work, that will be perfect for your family.
It must be hard to know what he had before the illness. I think he is cognizant of the changes and he may feel like there is little he can control right now. He can control his words. They seem to cry out in anger. Understandable so. Prayers for him and your family. If you can have him listen to the Book of Mormon daily maybe, he will receive peace from that activity. I taught Special Education for 12 years.
You have an incredible family.