The Chronic Phase: The Rehab Homestretch
The Social Worker at Primary Children’s Hospital told us that writing in a journal can be therapeutic. Even more, perhaps sharing our journey these past few weeks may help other families with children who suffer from this rare, devastating syndrome (F.I.R.E.S. = Febrile Infection-Related Epileptic Syndrome) or other chronic conditions.
I stopped including his seizure count because he hasn’t had any seizures since September 10th. His seizure control has been very good, but at the same time, the seizure medicines seem to be making him more sleepy.
Rehab Team, Day #23 (Saturday, September 30th)
93 days since onset.

Morning physical therapy session. Drew’s legs are a lot stronger than the first time he rode the bike on September 1st and he could only go across the bridge and back. Now he is riding around the parking lot loop.
5:30 PM: Drew was able to get all of his therapies finished by lunchtime, so in the afternoon, we went to Grandma Olsen’s on his Ride Pass today. We worked on stairs into the house, sitting balance, walking, and visiting with family. Because he is still on the Ketogenic diet, we had to pack his afternoon snack and we planned to return to the hospital by dinnertime.
Rehab Team, Day #24 (Sunday, October 1st)
94 days since onset.

The weather was sunny but cool and this was Drew’s first time walking across grass (he needed a lot of help). Sometimes Drew flips his eyepatch up when he doesn’t want to use it.
7:30 PM: Drew slept through most of the morning session of General Conference, but that was OK because we wanted him to rest up for another Ride Pass to Grandma Langford’s house in the afternoon. After he finished lunch at the hospital, we checked Drew out and drove to Grandma’s. Once we arrived, we went straight to the backyard and Drew tried shooting some baskets on the basketball court and he walked around a little bit on the grass. He was convinced he could do it by himself and kept trying to run or get up on his own but he nearly fell multiple times and we had to sit by him and watch him close. Once the afternoon session of General Conference started, we went inside for the rest of the time. He was able to pet the cat and some bunnies. He visited with many of his cousins, and his girlfriend even came over for a little while. The entire stay went well right up until he tried to eat dinner (which we brought from the hospital) and then there was too much commotion and distraction and he struggled to eat. He was also very tired and started to become agitated just before we left as he started yelling and saying mean things to people. We had to leave to return to the hospital and he could not hear what we were saying very well and he couldn’t understand why we had to leave back to the hospital. Otherwise, it was a good visit.
 Rehab Team, Day #25 (Monday, October 2nd)
Rehab Team, Day #25 (Monday, October 2nd)
95 days since onset.
11:30 AM: Drew talks a lot in his sleep, and I don’t think he did prior to getting sick. Sometimes you can tell what he is dreaming about — a couple of nights ago, he dreamt he was at the Lagoon amusement park with some friends. Last night he was talking to his brother and friends in his sleep. This morning when the nurses came to empty his bladder at 6:00 AM, he said, “Oh, that’s my favorite color.”
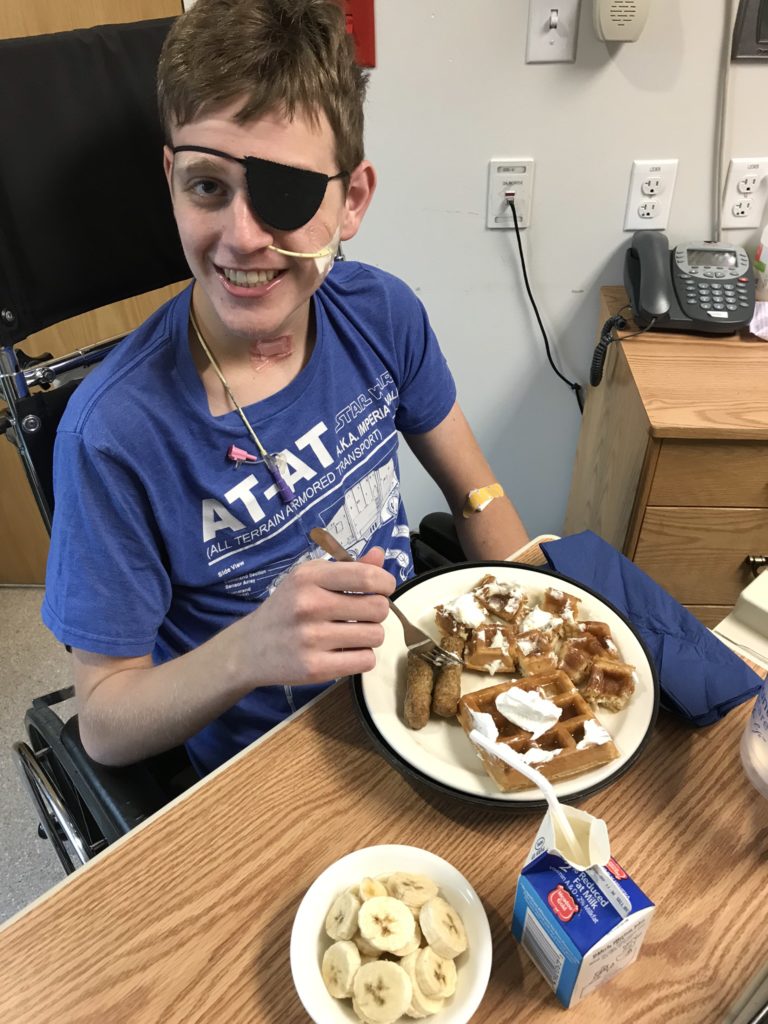
First day on a normal diet!!! Breakfast ended up being a little late because the doctor had to write the order first to advance to the normal diet, and then he actually got to choose what he wanted for breakfast from the menu. When the kitchen staff brought his waffles and sausage, Drew said, “I am so happy right now.” No more heavy-cream smoothies or chunks of butter and fat to eat!
The last several days, it seems Drew has been getting more sleepy after taking his morning seizure medicines at 8:00 AM. The medicines take about 40 minutes to kick in and then he becomes super sleepy and fell asleep multiple times during his morning therapy sessions. So this morning, the doctors switched his medications to 9:00 AM and then scheduled OT at 8:00 and PT at 8:30, so he did awesome in his morning therapies before getting sleepy from his medicines. Much better therapy sessions today.
In fact, during the afternoon OT session, they played a game of Blokus and he tied the therapist. We have noticed that Drew can still read, reason, and remember, but it takes him longer to do things. It seems as though the old Drew is returning, but his brain is stuck in first or second gear and he cannot shift and go faster yet. He can do a lot of things, but it just takes longer for him to process and think through things, and he definitely cannot be distracted or he gets sidetracked really easily. Considering how far he has come this past several weeks, we are happy with his progress and hope it will continue over the next several weeks.
Rehab Team, Day #26 (Tuesday, October 3rd)
96 days since onset.
The doctors changed out his air mattress/dolphin bed yesterday afternoon to just a regular bed, and last night and this morning, he could sit up without help (standing still needs help for his balance). He talked a lot in his sleep last night again, and then this morning, he was dreaming we were at church and he thought he was in a white shirt and tie. He was asking me if we were still in the Sycamores 4th Ward and if we still met at the “small Stake building.” He then started asking me if they were building more in the Sycamores and if they might build a bigger Stake building. He kind of remembers things, but I was trying to keep him going on his breakfast. He ran out of time to finish his French toast this morning (he ate about 3/4 of it).
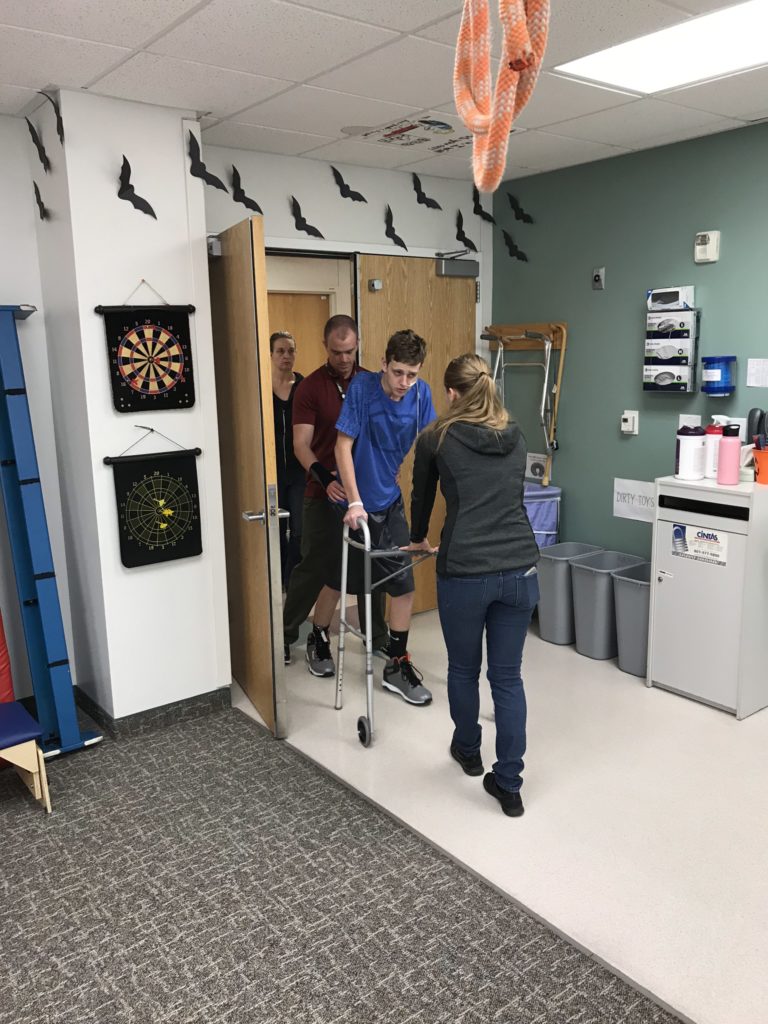
Usually, every Tuesday is the Rehab Team Conference where they discuss the patients’ progress and plan, however, due to some mandatory computer training, the Team Conference was pushed to tomorrow. Still, every Monday and Tuesday, the nurses and therapists have to assess how Drew is progressing with some of his tasks, such as his shower last night, and then this morning they had him try to negotiate a flight of real stairs. He actually did surprisingly well, but he needed to be verbally cued to look down at where he was putting his feet. He has the strength to do the stairs, but his balance is horrible and once he saw me taking pictures, he had a hard time focusing on the stairs and he needed more cues. He really has a hard time getting distracted whether it’s eating or therapy or anything and he really can’t do two things at the same time yet.
Rehab Team, Day #27 (Wednesday, October 4th)
97 days since onset.
Drew seems to be doing much better at night now, at least with staying asleep. His oxygen kept dropping last night as the nurses would try to turn it off, so finally the nurses left him on some supplemental oxygen (only 1/2 liter) and we may need to have him wear some oxygen at night when he goes home. He had pancakes and sausage for breakfast and did pretty good eating in time before OT started at 8:00 AM, but he really gets side-tracked easily and he barely got dressed and teeth brushed in time for PT at 8:30 AM. Then in PT, he was being kind of a stinker and kept saying he was “tired” and not listening to the directions of the PT. They are trying to work on his core strength and balance with crawling and kneeling exercises.
So we just finished meeting with Drew’s Rehab doctor. He is scheduled to discharge from the hospital on Friday, October 13th. We have a pass for this weekend and can take him home so long as we think he will be OK to return to the hospital (not sure). We have a lot to coordinate once we leave the hospital as he will need to follow-up with the following teams of doctors: Neurology, Rehab, Rheumatology, possibly ENT, Wound, Urology, Opthamology, and his Primary Care doctor, plus he will start home school and have his continued therapies which we are hoping the insurance will cover through Rehab Without Walls. They are going to purchase him a wheelchair as he will likely require it for several months. The doctors are not sure if Drew will be ready for BYU by next year, but hopefully in a year or two depending on his recovery and progress. Lastly, they hope they can remove his feeding tube before he leaves, but he has to be able to swallow all of his medicines/pills and consistently eat enough calories and drink enough fluids. Also, Dawn and I need to get trained on how to care for all of Drew’s continued medical needs, such as crushing his pills, caring for his tracheostomy fistula and his bed sore, and helping him empty his bladder. Needless to say, we have a lot of work to do before we leave, but we are all excited and looking forward to Friday, October 13th.
9:30 PM: Today the speech therapist and nurses started working with Drew on swallowing his pills instead of crushing and administering them through his feeding tube. In order to make sure he is swallowing the pills without chewing them, they gave him the pills one by one along with water or yogurt to help them go down better. Unfortunately, because of how many pills he has to take, it took him 40 minutes this morning to take his pills. Tonight, it took him nearly 45 minutes to swallow his 17 pills. The nurse is going to try and change some to liquid tomorrow and figure out how to speed up the process.
Rehab Team, Day #28 (Thursday, October 5th)
98 days since onset.
He did well this morning but seemed a little sleepy the last 2 days. I think he has gone to bed a little later and not had very long naps in the daytime, so he had a harder time waking up this morning. They mixed some of his pills into a liquid so he only had to swallow 4 pills and his morning medicines went a ton quicker. OT is trying to get him to speed up with his dressing and teeth brushing, but it still took him 22 minutes today. PT worked on crawling and core strength in the morning.
2:30 PM: Dawn sent me a text to call her as soon as I could, so I stepped out of my meeting at work and called her back.
”I just wanted to let you know,” she told me, “that we can’t wake Drew up this afternoon.”
”What?” I asked.
“He fell asleep about 10:00 this morning after getting his morning medicines, like he usually does,” she explained. “But we couldn’t get him to wake up for lunch and we still can’t get him to wake up now. He has missed all of his afternoon therapy sessions.”
“Do they know why?” I asked.
”The doctors have ordered some blood work and tests to see if they can find out what happened.”
”Is he having seizures again?” I asked.
”No, the doctors and nurses have checked several times and he is not having seizures. In fact, they can wake him up a little but and he will talk to us for a minute, but then he falls right back to sleep.”
9:00 PM: Drew finally woke up about 3:45 PM and acted like he usually does. He was able to wake up for a strawberry shake, Music Therapy at 4:30, and then the usual dinner and evening activities. When I arrived at the hospital, many of the labs had already come back and everything was normal. No signs of any infections. His Phenobarbital level was within his target range. The doctors had no idea what caused the long nap. It was scary, but perhaps he was just tired from all the hard work he has been doing?
Tonight his girlfriend came up to the hospital and we thought we would play a game. Unfortunately, all of the games in the Family Break Room were missing pieces. As a last resort, we thought we would let him try to play the X-box that is in each patient’s room. His vision had improved slightly the last few days as he could read some of the smaller words and pictures on the wall across the room. I went down to the nurses’ station to check out an X-box game, but his first choice (Call of Duty) was already checked out. I ended up checking out the Legos Marvel game for him. We don’t have an X-box, so he had a hard time working the controller at first, but with his girlfriend’s help, he eventually got it and they played the game for a little while. He couldn’t really follow the directions on-screen or understand fully what was going on, but it was worth a try.
Rehab Team, Day #29 (Friday, October 6th)
99 days since onset.
This morning, we helped take Drew down to the Radiology department to get an ultrasound of his kidneys and bladder. With his difficulties emptying his bladder and his previous CT scan showing some inflammation in his kidneys, the doctors wanted to make sure his everything was OK.
In the afternoon, Drew’s brother and older sister came up from Provo to visit. Drew has such a busy schedule, and because he gets distracted so easily, there wasn’t a lot of time for them to visit. But they got to spend a little while with him after all the therapies were finished.
© Copyright 2017 Jeff, All rights Reserved. Written For: Jeffrey Olsen




So happy for all the little wins! They all add up to progress and Drew coming home!
Bravo, Drew! I see many blessings for your family! Praying you’ll continue to find solutions & support!