The Sub-Acute Phase: Baby Steps
The Social Worker at Primary Children’s Hospital told us that writing in a journal can be therapeutic. Even more, perhaps sharing our journey these past few weeks may help other families with children who suffer from this rare, devastating syndrome (F.I.R.E.S. = Febrile Infection-Related Epileptic Syndrome) or other chronic conditions.
Neuro Floor, Day #9 (Saturday, August 26th)
58 days since onset. Seizure Count = 5 Focal Seizures today.
7:30 AM: “Drew, your bladder is full,” I told him after the nurse finished scanning his bladder with an ultrasound. “Can you try to go to the bathroom?”
“I don’t have to go right now,” Drew said. He has not regained full sensation and he continues to have weakness and limited motor control throughout his body, so we’re trying to practice and facilitate his bladder muscles.
“Drew, if we don’t try to go to the bathroom,” I explain to him, “then the nurses will have to use a catheter because your bladder is full. Can you try to go?”
“I guess,” Drew shrugged his shoulders, “but I really don’t have to go.”
I helped Drew sit up on the side of the bed. As he rolled and sat up, I held his head while he helped to pull his trunk up and then I helped swing his feet out of bed.
“Go ahead and count to 3, Drew, and then we will stand up,” I say as I stand in front of him, his hands on my shoulders, and my arms under his shoulders holding his trunk steady.
“One… Two… Three,” he said and then he leans forward and I help lift him to stand up on his wobbly legs. I held his trunk upright as he struggles to shift and pivot his feet, but then eventually he is lined up with the shower chair (which has wheels) and we slowly lower down onto the seat. I then rolled him into the bathroom, and we repeat the process to stand and pivot to the toilet. We have to shove a pillow behind him so he can lean back against the plumbing, and then he holds onto some grab bars on the wall to steady himself. Even still, either his mother or myself have to help him hold his head up, especially as he begins to fatigue.
Despite trying for several minutes, he cannot release his bladder to empty. As he becomes more fatigued and starts leaning, we reverse the process and get him back to bed before he is too tired to help us. The last thing we need is for him to have a seizure or fall and injure himself and prolong our hospital stay.
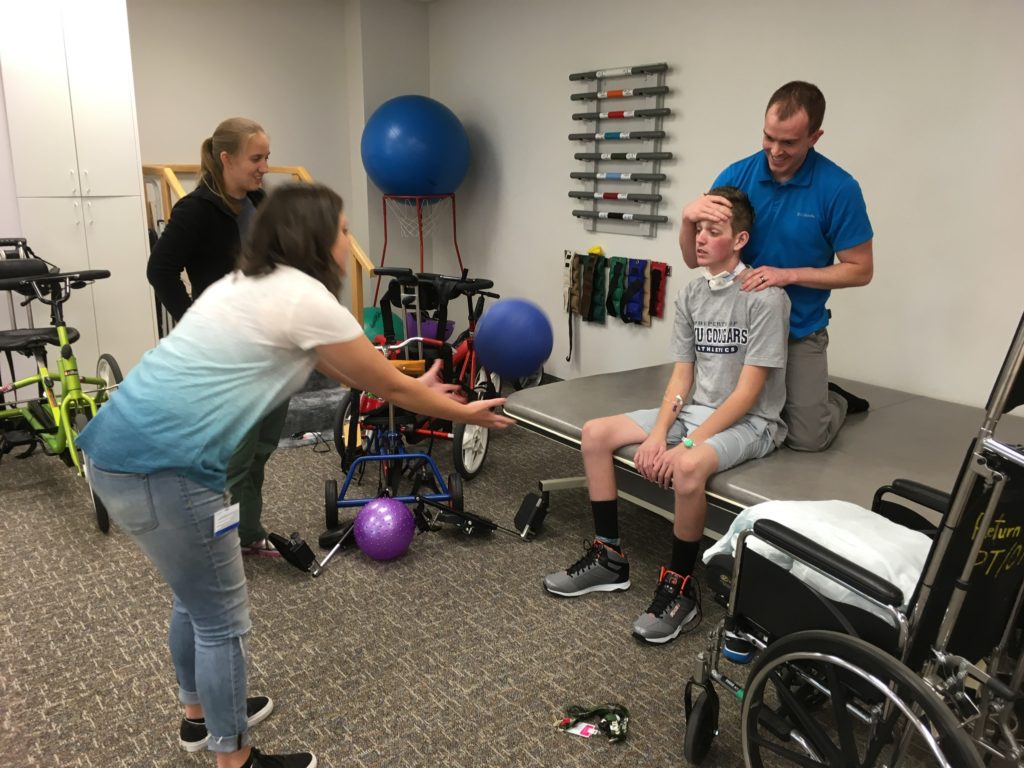
2:30 PM: We repeated the attempt at the bathroom three more times in the morning, but still no success. However, he was so tired from all of the transfers, he fell asleep and the PT and OT had to reschedule his therapy appointment from 10:00 to 2:00. We had to work to get him to wake up, but once he was awake, he readily agreed to participate. He worked with them on unsupported sitting and rolling on the mat, and then as an added bonus, he played catch with his girlfriend, M❤️❤️❤️❤️. He felt ready to have his friends visit, but we thought we better start small and make sure he didn’t freak out again. So M❤️❤️❤️❤️ came up this afternoon and not only did they have a nice visit, she helped inspire him to work harder in therapy.
Neuro Floor, Day #10 (Sunday, August 27th)
59 days since onset. Seizure count = 3 Focal today (one for 7 minutes)
5:30 PM: “I was asleep for 7 weeks and 3 days,” Drew told his friends from school. “I woke up on August 24th.”
I returned from my church meetings this afternoon to find Drew’s room full of visitors, mostly his aunts and uncles and grandparents, but he had his attention focused almost exclusively on three of his friends from high school.
“I need you to sign me up for auditions tomorrow,” he said to his best friend. “I won’t be at school tomorrow, but I hope to be able to make it in time for the auditions.”
His friends kind of looked at his mother and I wondering if this was true or not.
“We’ve told him he won’t make it to auditions,” his mother said, “But he keeps hoping they’ll figure out some way for him to go.” The auditions at the high school are for this year’s musical, ‘My Fair Lady.’
His friends did bring some of the sheet music for the audition, and they sat and sang with him a few bars of “On the Street Where You Live.”
A short time later, as his friends prepared to leave, his mother tried one more time saying, “Drew, you won’t be able to leave the hospital tomorrow for the audition.”
“I know,” he said. “That sucks.”
8:30 PM: This evening we got Drew into his wheelchair and took him for a ride out to the waterfall garden in front of the hospital, and while he was out there, he saw the parking garage and wanted to go see his car. So his mother and brother and sister rolled him out to his car for a few minutes and he looked at his old car. At least once per day, we try to go outside with Drew and take in some fresh air. Once he returned to his room, he was pretty tired, but he was still able to play catch with his brother for about 45 minutes. They would throw a soft football back and forth as they talked about remembering things like his address and movies and different things they used to do together.
This morning, the doctors said that they plan to start “capping” his tracheostomy tomorrow for a couple of hours. Each day, they will gradually increase the time his tracheostomy is capped and hopefully after a week or so, he will be able to get the tracheostomy removed. We continue to be very blessed with his progress and pray it continues at such an incredibly fast rate.
9:30 PM: “Can I have a hug?” Drew asked each one of his siblings and his mother as they prepare to go home. One by one, they lean over the rail of his bed and he grabs them with his arms and gives them each a hug and a kiss on the cheek.
Lastly, we resumed one other tradition to close each day with a family prayer. Since Drew is in the hospital, we gather around his bed with folded arms and bowed heads and say family prayer. Last night, he kind of watched us with his eyes open, as if he wasn’t sure what we were doing. Tonight, however, he closed his eyes and bowed his head along with the rest of us, and when his sister said, “Amen,” he said “Amen” as well.
Neuro Floor, Day #11 (Monday, August 28th)
60 days since onset. Seizure count = 1 Focal Seizure today.
9:30 AM: Drew’s mother arrived at the hospital just as the fourth team of doctors were finishing their assessment, and Drew looked exhausted, with slurred speech, half-open eyes, and delayed responses.
“I’m not sure what we can do to get him to sleep longer at night?” I asked. “He was so tired last night from all of his visitors that he fell asleep by 8:45 PM, and then he woke up this morning at 4:15 AM and has been awake since.”
“Are you sure it was 4:15 this morning?” She asked me.
“Yes, because he kept trying to pull all of his tubes out and the nurse assistants kept telling him to stop,” I said. “So I woke up also, and neither one of us has slept since then.”
“Well, that is going to make his physical therapy hard again,” Dawn said as she shook her head. The physical and occupational therapists have been trying to work with Drew each weekday at 10:00 AM, but about half the time he has fallen back asleep or is too tired.
“It doesn’t help that from 7:00 AM onward there are four different teams of doctors all taking turns examining Drew, as well as the nurses and respiratory therapy all coming in and doing assessments throughout the morning, asking him questions, testing his muscles and his memory, and so there isn’t much time for a nap until late morning when he is supposed to do physical therapy,” I said. “If only he could sleep until 7:00, that would be ideal, but not sure why he wakes up so early?”
Sure enough, by the time the physical and occupational therapists arrived at 10:10 AM, Drew had fallen back asleep and couldn’t wake up for them. They rescheduled to try back at 2:00 for his therapy session.
11:30 PM: So today, the doctors switched Drew from continuous feeding through his feeding tube to bolus feedings, which prepare him for a more-normalized routine to transition back to mealtimes. He continues to work with speech therapy on swallowing, but he is a ways away from trying to eat any food yet, especially on the Ketogenic diet (so we have been careful not to eat any food in his room in front of him). However, tonight was kind of a perfect storm and the result was him throwing up.
Drew was nearing the end of his dinnertime bolus feed when the nurse started to give him his evening medications through his feeding tube. We were also helping him to brush his teeth for bedtime, and as he was trying to rinse and spit, some of the water went down his windpipe and he started coughing. As he coughed, his gag reflex kicked in and he threw up all over his shirt. I quickly rolled him to his side and he proceeded to throw up all over his shirt and pillow. He threw up quite a bit, including half of his evening medicines. So after we got him cleaned up, the nurse had to go call the doctor and get orders to re-administer the medicines he threw up, and then pharmacy had to send them up again. Unfortunately, while I turned around to put his dirty clothes away, I turned back around to find that Drew had pulled out his IV (“I thought it was some dead skin,” he said). Finally, the nurses were able to give him the rest of his medicine and he was cleaned up and ready for bed, but it was pretty late and I couldn’t wait up for the IV Team to come give him a new IV.
Neuro Floor, Day #12 (Tuesday, August 29th)
61 days since onset. Seizure count = 1 Focal Seizure today.
9:30 AM: I talked to the doctors this morning about trying to figure out how we can get Drew to sleep better at night. After he threw up last night and pulled out his IV, we didn’t get to sleep until almost midnight. Then the nurses had to come in at 4 AM to give him his Anakinra shots (which still hurt a lot) and then at 6 AM to do a bladder scan and insert a catheter to help him empty his full bladder. Drew and I were both exhausted from lack of sleep and a steady stream of healthcare workers. As Drew gets tired, his speech and memory and attention definitely get worse. The doctors’ initial solution was to cut down on his daytime naps, but I told them we can’t cut down on naps until he is sleeping better at night. We’re both getting interrupted so many times, the daytime naps are a natural result (although I don’t get a nap because I have to go to work). After some discussion, they agree to consolidate all of his medicines and shots at 8:00 and to decrease the frequency of some of his vital signs and bladder scans.
5:30 PM: “Do you like my shoes?” Drew asks the nurse. He has already asked her this same question three times today, but either he can’t recognize her face or he has forgotten that he told her, so he is asking her again.
“Yes,” the nurse answers, “those are nice shoes.” She nods politely at his orange and gray high-top tennis shoes.
“These shoes are size 13 and they only cost $30,” Drew says as he points at his feet. “And can you believe they came from Wal-Mart?”
“No way,” the nurse says to him.
“Yes, Wal-Mart,” Drew said. “They are freaking sweet shoes.”
His brother turns to me and says, “You know, the old Drew would never buy shoes at Wal-Mart.”
“I know,” I replied. “After all he has been through, I’m glad to see him get excited about anything.”
Neuro Floor, Day #13 (Wednesday, August 30th)
62 days since onset. Seizure count = No seizures today.
11:00 AM: Drew walked today in therapy! He was unsteady and ataxic, but he was able to take 5 steps as I and his physical therapist helped him. His right arm and leg are definitely stronger than his left arm and leg (Which is why Neurology wants to do another MRI of Drew’s brain in the next week or so) and his trunk and neck muscles are still weak, but he was able to walk to his wheelchair at the conclusion of his therapy session this morning. His biggest challenge right now continues to be his sleep and getting some rest breaks during the daytime that don’t interfere with his therapy sessions.
8:30 PM: Drew was lucky to have three of his friends from high school visit this afternoon. They talked to him for quite a while, pulling up pictures on their phones and talking about school and friends and dances and normal teenager topics. After a while, we got him up to a wheelchair and they escorted him to the waterfalls and garden in front of the hospital. He was very tired, but no chance he was going to fall asleep with three teenage girls visiting him. One of them gave him a gift before leaving, and he was thrilled to see that she gave him a “Star Wars” fleece blanket.
Of course Drew did not make it to auditions yesterday for the high school musical, but his mother emailed the director and asked if Drew could still take part in the ensemble. Based upon his amazing progress, we are hopeful he can still participate to some extent with the musical when it is performed in November. The response was a resounding ‘yes’ and not only that, there were several tributes to Drew throughout the auditions as he was missed. We are so grateful to the faculty, staff, and students at Copper Hills High School for their wonderful support and encouragement. The director sent us the sheet music for the songs and the Music Therapist and his mother will start helping him learn the songs next week. Even though it is not one of the leads, he is really excited to be able to still take part in “My Fair Lady.”
9:30 PM: “Is it OK if we have family prayer before we go home for the night?” Drew’s mother asked.
“Sure,” Drew said.
“I think it’s your turn, Drew,” I said. His younger sister was at work, and his brother was out with some friends, so it was just Dawn, Erin, and myself. “Do you think you can say the prayer tonight?”
“Sure,” he said. “Everyone close your eyes.”
He paused and waited for us all to fold our arms and close our eyes, and then he started, “Heavenly Father…. We thank thee for the day we had today….” In the end, he gave a short, but sweet prayer that left us all crying, especially as he asked for continued healing and progress from his seizures. As his mother and sister departed, there was a sweet spirit in the room that lingered long after the prayer finished.
Neuro Floor, Day #14 (Thursday, August 31st)
63 days since onset. Seizure count = No seizures today.
9:00 AM: “I can see a little better today,” Drew said.
“Really?” I asked. “Tell me what you can see on your wall…”
The wall opposite his bed is decorated with cards, posters, and pictures.
“I can see the big letters along the top that spell ‘We ❤️ DREW,” he said. “I can also see there is a red octa… shape with black letters in it.”
“You’re right, Drew,” I nodded. “There is a ‘STOP’ sign with some words in it.”
He proceeded to read some of the bigger letters and shapes, such as a large card with a heart and his name in it, but many of the smaller letters and words were blurry. He said he could mostly just see colors and blurry shapes, but not the details.
2:45 PM: Unfortunately Drew was asleep when the PT and OT team stopped by in the morning, but they rescheduled for this afternoon and it was worth the wait. They helped him onto a three-wheeled bicycle and then took him for a ride across the bridge that connects the hospital with the outpatient office building. He loved it. He struggled at times to hold his head up and sit tall, and he kept veering to the left because his left arm is weak, but for the majority of the ride he powered the bike and steered it himself. After he finished, his left leg and arm were visibly shaking from the exertion, but Drew hardly noticed.
8:30 PM: As the University of Utah football team played their first game of the year tonight, we worked our way through the crowd and traffic back up to the hospital to find that we had just missed two of Drew’s co-workers from his job at the Kearns Fitness Center. They brought a bundle of cards from his other co-workers, along with a stuffed monkey in swim trunks to remind him of work. He loved it. Initially, he did not recognize them, but as they talked, he quickly remembered them and started asking all sorts of questions about the staff, the remodel project, and other details about work. After they finished, he was elated that they stopped by to wish him well.
Drew called him “Super Monkey” because he thought he had a cape, so we converted the monkey’s shirt to a cape.
Neuro Floor, Day #15 (Friday, September 1st)
64 days since onset. Seizure count = 2 Partial seizures today.
8:30 PM: Another bike ride today in therapy, and Drew was loving it even if the pedestrians on the bridge to the outpatient building were not. I spent the day trying to help Drew’s brother fix a car for him to take back to school to Provo, so I wasn’t around as much during the afternoon, but his mother said it was a good day overall.
However, in the evening, we were struggling to keep Drew awake long enough to make an attempt at using the bathroom and taking a bath. He was so incredibly tired after his therapy and visitors and did not have a nap since the morning, so his speech was really slurred and his eyes were half open. To help him stay awake, we played catch with a nerf football with him. He can throw the ball pretty hard and accurately with his right hand, and he can catch it most of the time if it goes into his lap. We tried to keep him talking and throwing until the nurses were finally finished with their shift change and ready to help (also, the nurse was trying to get all of Drew’s medicines first, which delayed his help as he has to crush them and dissolve them all in water for his feeding tube). It took maximal effort to get him to the toilet, but within minutes of sitting down, he fell asleep and could not be woke up. It took me and the nurse and his mother all lifting him to get him back to bed, and even still, we barely got him there. From what I have researched, 50% of patients with brain injury have sleep disturbances, both in sleep initiation and sleep maintenance, and yet sleep and mental rest are critical to recovery from a brain injury. We continue to try and work with the nurses to figure out a schedule for Drew to help him improve his sleep.
© Copyright 2017 Jeff, All rights Reserved. Written For: Jeffrey Olsen



Thank you so much for these updates. I have been following Drew’s progress for quite some time and am amazed at the improvement in recent weeks. Your faith and upbeat attitude throughout this have truly been an inspiration to me. My hope and prayers are that Drew will continue toward a complete recovery.
Looks like you are beginning to make measures in feet instead of inches for progress. It is hard to imagine he has spent most of the summer in the hospital. Are you, his parents doing well? Are you loosing weight and feeling shut off from the real world. Many prayers going your way, and we will put his name in the St. George temple this week.
Such wonderful news!❤️ So happy for Drew, the family and his friends!😊
Keep the updates coming! You are all in our prayers!
So wonderful to read of his progress! Praying for him everyday…
I have tears in my eyes reading this. Keep going, Drew!
I am happy to see that Drew is doing better. My prayers are with you all. May the Lord Bless You and Keep you all. 😊 prayers, Darlene Drake
My daughter is in the same grade as Drew and my older son is the same age as Alex. I pray for all of you as you go through this. Life can seem cruel at times. I was bursting with tears when I read about the play! How wonderful! I plan to be in the audience to chear him on! Bravo Drew and family❤️The Browns
LaMar & I just finished reading the latest progress about Drew. We love the pictures and are so grateful he is doing so well. Our continued prayers for Drew. Miracles happen even today! 💓