The Acute Phase: The “Miracle Boy”
The Social Worker at Primary Children’s Hospital told us that writing in a journal can be therapeutic. Even more, perhaps sharing our journey these past few weeks may help other families with children who suffer from this rare, devastating syndrome (F.I.R.E.S. = Febrile Infection-Related Epileptic Syndrome) or other chronic conditions.
“I believe there’s an inner power that makes winners or losers. And the winners are the ones who really listen to the truth of their hearts.” – Rocky Balboa
Neuro Floor, Day #3 (Sunday, August 20th) — 52 days since onset
5:00 PM: “What do we have to do?” Drew mouthed to me when I returned to the hospital after church.
He was lying in bed with half-opened eyes, surrounded by the rest of the family. I wasn’t entirely sure what he was saying, “Are you asking me what to do?”
“What do we have to do?” He repeated. This time his mother helped me to read his lips.
“We have to work on getting stronger and get better,” I answered.
“What do we have to do?” He asked again.
“We will work with therapy the next few weeks, and then we will get strong enough to go home.” I explained more slowly.
Drew shook his head in frustration. “Do you hate me?” He mouthed.
“Of course we don’t hate you,” I shook my head.
“Do you hate me?” He repeated.
His mother leaned in close to his bed, “We love you very much, Drew.”
“Do you hate me?” He looked like he wanted to cry.
“No, Drew,” I said. “We love you very much.”
I don’t think he understood.
8:00 PM: “Tell them to go,” Drew was mouthing to us as he repeatedly waved his hand toward the door.
M❤️❤️❤️❤️ and her parents had stopped by in the evening to visit, but Drew surprised us when he became upset and angry.
“Drew, be nice to them,” I said. “They drove all the way up here to see you.”
“Tell them to go,” Drew repeated. He closed his eyes and shook his head as he continued waving for them to leave.
“Drew, why don’t you want them to visit?” I asked.
He kept his eyes closed tightly and kept shaking his head no.
“Do you not want them to see you?”
He continued to shake his head no.
“Do you not want them to see you? Are you worried what they might think?”
Drew nodded his head yes. Despite any and all reassurances, Drew would not calm down and would not visit with them, so his visitors slowly filed out of the room and wished him well. Tears came to my eyes as I realized he was finally starting to became aware of his sickness and his condition.
“OK, Drew, you tell us when you feel you will be ready for your friends to visit.”
In the end, I suppose we have had 7 weeks to process and grieve, and now that he is finally waking up, Drew is starting to go through the same emotions as he processes how much his life has changed due to his illness.
Neuro Floor, Day #4 (Monday, August 21st) — 53 days since onset
8:30 AM: After such a traumatic and emotional evening, Drew woke up in a better mood this morning. He would mouth to us that he was “A-OK” and flash us an OK sign with his hands and fingers. However, he did not remember where he was and I had to remind him he was still in the hospital. He still has not moved his legs much and is only showing a flicker of muscle movement in his thighs.
1:00 PM: Unfortunately, Drew’s feeding tube clogged this morning and the nurses worked for nearly an hour to unclog it, but in the end, they had to pull the old tube out and insert a new feeding tube. The process is rather uncomfortable as they thread the tube up through one of his nostrils and then down the back of his throat to his stomach. He squirmed and winced the entire time. Once they had it threaded, Radiology came and took an X-ray to check its placement. As a result, the morning medications were a few hours late, and he became really sleepy when the therapists came into the room to work with him.
7:30 PM: “Dad, do you remember where you parked our car?” Drew asked me as I entered his room. I was shocked to actually hear his voice — although it was raspy and barely audible.
I walked over to his bed and leaned in close. “Why, yes, Drew, I remember where I parked our car, but we can’t leave the hospital right now.”
“The Respiratory Therapists put in a smaller tracheostomy cannula this afternoon,” Dawn explained to me. “The smaller cannula will help him to wean off of the tracheostomy by building up his lung and diaphragm muscles. It will also allow Speech Therapy to put a valve on the end of the cannula to allow him to speak.”
“Dad, do you remember where you parked our car?” Drew asked again.
“Yes, Drew, I know right where I parked,” I answered. Then to his mother, I said, “sounds like he doesn’t need a valve to speak.”
“His lungs are strong enough that he started speaking to us tonight without the valve,” his mom said.
9:15 PM: As his mother, sisters, and brother were preparing to leave for the evening, Drew asked in his breathy, raspy voice, “When do I get to go home?”
“We’re not sure,” his mother answered. “We love you very much and will be back in the morning.”
“When do I get to go home?” He asked again.
“Soon, Drew,” I said. “Soon….”
Neuro Floor, Day #5 (Tuesday, August 22nd) — 54 days since onset
5:30 AM: I was awake most of the night watching Drew because he kept trying to pull out all of his lines and leads. He doesn’t even realize he is doing it most of the time, but just feels the tape on his skin and tries to pull it off. He nearly got his feeding tube out a couple of times, and he had such a hard time getting it replaced, I didn’t want to see him go through that again.
9:00 PM: Drew has been talking a lot today — with and without the valve on his tracheostomy. As he has been talking, we realized he has had difficulty remembering words and names. He even had to be reminded of his brother’s and sisters’ names. He worked with physical therapy today in the rehab gym and practiced sitting on the edge of the mat for about 15 minutes. He also worked with speech therapy and swallowed some sips of water and ice chips, but it was difficult for him to consistently direct the water down his esophagus and not his wind pipe. His mouth and throat muscles are just as weak as his legs and arms, but the doctors have been so impressed with how much he is progressing, they said he may be ready for the full rehab within two weeks so long as his seizures continue to remain stable. We started tracking his seizures to monitor the effectiveness of the medications, and he was down to only about 12 seizures on Sunday, then down to about 6 on Monday, and then only 4 so far today. Overall he has come a long way in only 6 days, but still a little way to go. I am sure Drew would have much rather been in school today.
Neuro Floor, Day #6 (Wednesday, August 23rd) — 55 days since onset
11:00 AM: Unfortunately, Drew had a seizure about 20 minutes before the physical and occupational therapists came in to work with him, so he was kind of sleepy and tired in his post-icthal state. They were able to get him up to the cardiac chair and then both therapists helped him to slide from the cardiac chair over to the mat in the corner of the rehab gym. The gym is a large, open space with mirrors, white walls, white cabinets, three mat tables, and various other pieces of equipment, such as adaptive bicycles, practice stairs, and swings. The therapists have been working with Drew on unsupported sitting, kicking a ball, throwing a ball, rolling, and lying prone on the mat.
Noon: Drew just finished working with the speech therapist. She was able to attempt feeding him with some Ketogenic-friendly sour cream that had been dyed blue. Drew did great with the first two swallows, but the third swallow, he kind of inhaled as he tried to remove the sour cream from the spoon. He sat for a couple of minutes with a stunned look on his face as he realized something wasn’t right, but he couldn’t figure out what to do. After the speech therapist coached him on clearing his throat and coughing, it seemed he was able to redirect the sour cream. However, a minute later, he coughed again and blue foam came out around his tracheostomy.
5:00 PM: Drew’s favorite part of the day is Music Therapy, and today he sang along with the speech therapist for the first time instead of just listening. The songs are simple and familiar to help the patients remember, such as the alphabet song and nursery rhymes, and even still, he would often echo the words and need frequent prompting to remember the words.
9:30 PM: “I heard he’s talking now?” One of the Respiratory Therapists from the ICU poked his head into Drew’s room. He worked with Drew a lot while he was in the ICU, but he had been on vacation for the past week and had not seen Drew since the ICU.
“Drew,” I said, “can you say ‘hello’?”
Drew smiled and waved his hand toward the door, and then he said, “Hello….”
“Are you kidding me?” The Respiratory therapist about fell over. “He could barely move his arms, and there was no way he could talk a week ago, and now look at him!”
For the next several minutes, Drew met someone who took care of him while he slept, and the therapist left flabbergasted. Earlier in the afternoon, one of the ICU doctors who saw Drew on his second day in the ICU stopped by, and she left in tears as he talked to her. As we shared all of the progress Drew had made, the doctor hugged Dawn and they cried for a few minutes together.
Neuro Floor, Day #7 (Thursday, August 24th) — 56 days since onset
11:00 AM: Drew stood up for the first time! In fact, he practiced standing 6 times as he got into and out of a wheel chair twice. Toward the end of his physical and occupational therapy treatment this morning, the therapists put together a reclining wheelchair for him to use. He stood again with both therapists and pivoted to the wheelchair to return to his room, and then back to his bed, but it took max assist from both of the therapists. During his therapy sessions, he also practiced sitting up on the edge of the bed several times.
5:00 PM: This afternoon Drew practiced writing letters and words on a dry-erase board with his sister’s assistance. He still has trouble reading small letters and his handwriting is difficult to read because he still has some ataxia and weakness in his hand, but he was getting better at reading words after his sister would write them out. Unfortunately, he worked so hard on his reading and writing, his afternoon Speech and Music Therapy treatments were kind of a disaster because he was so tired and mentally drained. As he gets tired, his response time slows and his words become more slurred and delayed. He did have about 5 seizures today, but overall had a good day and he continues to work on his memory and talking.
We felt bad missing another family function today — our neice got married in Utah County today, but it just rips our heart out to go to a family function with Drew in the hospital. Our family is not complete, so it is difficult to celebrate or leave him behind. We hope they understand and know that we will congratulate them in person, and with our whole family, in a few weeks.
8:30 PM: “Dad, where’s my phone?” Drew asked.
“It’s on the table next to your bed,” I said.
“Dad, can you give me my phone?”
I handed him the phone, and he studied it for a couple of minutes, trying to swipe the screen and struggling to read any of the numbers or letters. Finally, he held the phone back out to me and asked, “Dad, can you dial M❤️❤️❤️❤️’s number for me?”
I searched his contacts and dialed the number, and then I helped him lift his arm so he could hold the phone to his ear. Even though he has been moving his hands and elbows, his shoulders are still very weak, especially his left arm.
I smiled as he talked to his girlfriend about the first couple of days of school and choir, because school started two days ago. She patiently described to him what he was missing, and that he was missed.
Also, a couple more nurses and staff from the ICU stopped by after shift change this evening to see for themselves how well Drew was doing. They could hardly believe it was the same boy.
Neuro Floor, Day #8 (Friday, August 25th) — 57 days since onset
7:00 AM: Unfortunately, Drew pulled out his feeding tube this morning. The nurses spent 45 minutes getting a new one inserted. Once they finished, Drew was talking up a storm.
“Did I start school yesterday? What time is it?” Drew asked me.
“There’s a clock on the wall,” I pointed. “Can you tell me what time it is?”
“I can’t see the numbers,” he said.
“Well, it is a few minutes past 7:00 in the morning.”
“I’ve got seminary at 6:00,” Drew said with an alarmed look on his face. “Then I’ve got Drama, and Choir, and BC Calculus,…”
For the next little while, Drew was remembering his class schedule and talking all about A-days and B-days and how much he wished he could be at school. One of the big concerns that he kept mentioning was the auditions for the school musical coming up next week on Monday and Tuesday. He is convinced he will be there, and he plans to call his friends to sign him up for a slot.
5:30 PM: One of the nice features of being able to get up to a wheelchair is that it has wheels. After he finished his afternoon Speech and Music Therapy session, the nurse agreed to accompany us on a walk to go to the outdoor garden on the third floor. Because of Drew’s tracheostomy, the nurse must accompany us with a bag full of emergency items in case Drew’s tracheostomy falls out or becomes clogged. We sat for nearly 30 minutes in the shade of the patio garden, looking at the various statues and potted plants. The whole time Drew was nervously looking at his phone as he had asked me to send some text messages to some of his friends. He was having a hard time patiently waiting for their response and wanted me to send the messages again.
On our way back into the hospital, I noticed Drew was struggling to breathe. “Drew, are you OK?”
His face was bright red and he was making a strange sound from his throat as he gasped and struggled to take in a breathe. The nurse had a look of alarm cross her face and called Respiratory Therapy on her walkie talkie badge as we raced down the hallway back to his room.
Once in his room, the nurse grabbed the suction from the wall and started to try and help remove whatever was blocking his airway, but was having little success. I helped the nurse by hooking up the pulse oximeter to his finger while she worked on his tracheostomy.
“Fortunately,” I noted, “his Oxygen is good at 93%.”
Still, he was gasping and trying to cough something out of his airway. Respiratory Therapy made it to the room and they are able to suction a little deeper, but he also had little success.
“What I think may have happened,” the Respiratory Therapist said, “is that he has been on the speaking valve a little too long today and the lack of humidity with the valve and the outside air has dried out his secretions to the point that he cannot clear them.”
The Respiratory Therapist pulled off the speaking valve and flakes of dried secretions came falling out, but Drew still worked to clear something out of his airway. The Respiratory Therapist placed Drew back on the tracheostomy breathing mask, which gives him humidified oxygen to breathe. “Let’s have him breathe with his mask for a while and moisten back up his airway.”
I then helped the nurse to stand Drew and pivot him back to the bed as he looked extremely pale. We laid him down and positioned him, and fortunately all of his vitals looked good. It took about 30 minutes on the humidified oxygen for his secretions to moisten enough for Drew to finally cough them out.
8:00 PM: Drew’s seizures continue to be well-controlled, with only 4 to 8 seizures per day this past week, although one day he only had 2 seizures. They have all been partial seizures affecting primarily his eyes, mouth, and twitching of his hands or shoulders. One of the new doctors told me that the way one of the Neurologists described Drew’s brain waves on the EEG had been that he was having “seizures on top of his seizures,” and now the anti-seizure cocktail seems to finally have brought them under control.
9:00 PM: “I don’t know if you remember me,” the new Respiratory Therapist said as he entered Drew’s room and started writing his name on our dry erase board. “I took care of Drew a couple of weeks ago in the ICU, and I will be taking care of him again tonight.”
Drew smiled and waved at the therapist. “Hi, I’m Drew.”
“Wow,” the therapist smiled. “So what they are saying really is true. The ICU staff started calling him the “miracle boy,” and I wouldn’t have believed him to be the same boy I cared for in the ICU unless I saw it with my own eyes.”
I never could understand why the Case Managers were researching long-term care facilities to place Drew into after the hospital. In my mind there was no doubt he would be going to rehab and walking out of the hospital, so it was frustrating early on in the process when they would ask us to choose a facility for him. Whether it was our conversations with other FIRES families, or simply our belief in Drew’s motivation and strength, we knew he would “wake up” once the seizures subsided, and although he still has a lot of hard work ahead of him, he has come back to us.
© Copyright 2017 Jeff, All rights Reserved. Written For: Jeffrey Olsen


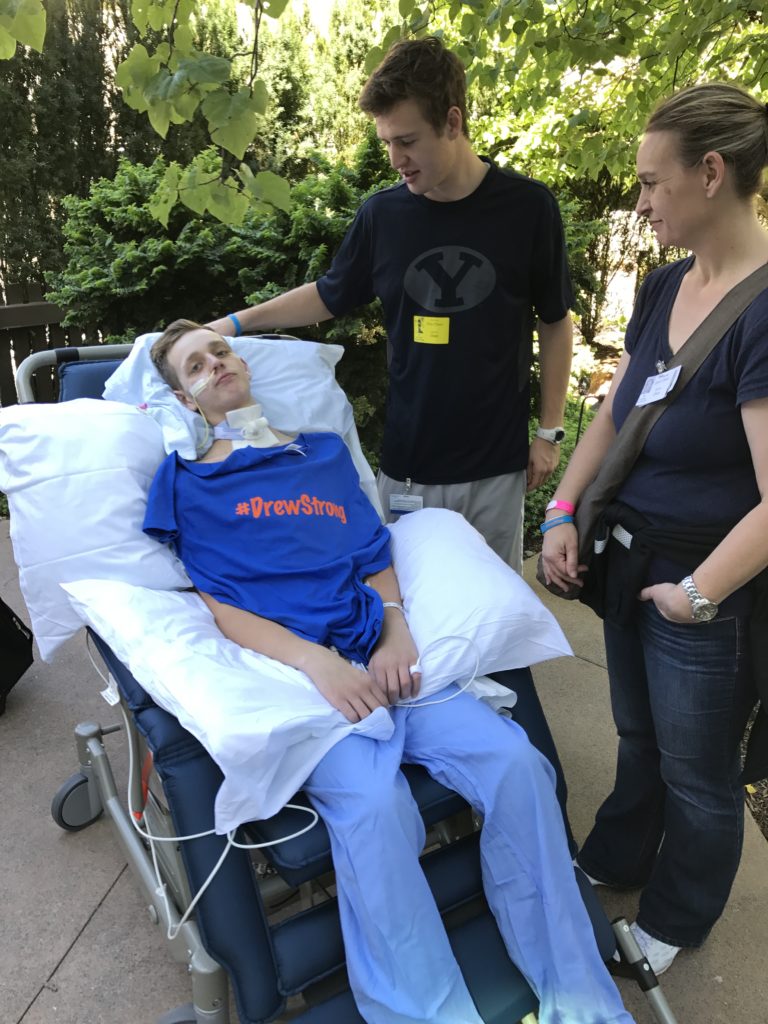
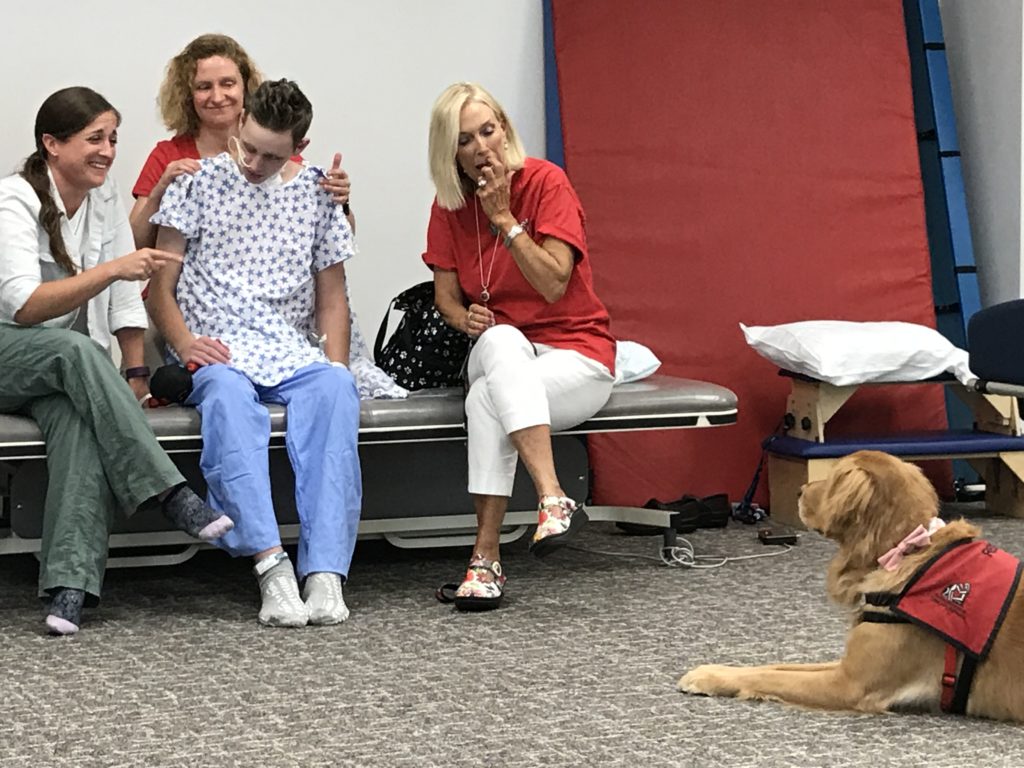
So thankful. I know it is still a lot of work ahead, but he is the miracle boy. Love you all.
Aunt Carol
Prayers are answered. He truly is a miracle. Love to your family and continued prayers.
Awwww I’m just in tears I’m so happy for drew and you and your family, praise god!!! Thank you lord for hearing our prayers and responding to our faith in you xoxo
I don’t know your family but I have found myself thinking of Drew and all of you often. I truly wish Drew the best and hope you will continue to update us. Yay Drew!
What an amazing young man! Your family’s strength is truly inspiring. He definitely is a miracle!
My daughter is friends with a young lady who goes to school with Drew and has known him since they were younger. She is the person who told me about Drew many weeks ago and I have been reading your blog ever since. There were times I cried after reading a new entry. I thought about him last week when school started. I have prayed for him, for your family and friends every day. Now I am crying for a different reason. I am so thrilled that he is doing so well! I have to say I never doubted that he would recover and not need a long term facility. I will continue to pray, continue to read your blog and look forward to the one that announces when he goes home!
You don’t know me, but I have been following Drew’s story and have been praying for him. It makes me so happy to hear of his progress & I wish him the best throughout the remainder of his recovery.
Good job Drew, Jeff, Dawn and family!! 😁 What a great miricle!! ❤️We’ll keep sending prayers your way. 🙏🏼
Jeff,
I am so glad your son is doing so well after all of those weeks of uncertainty. Thank you for writing this blog. I am sure that it will be so helpful to other families and the medical community. You probably were faced with one of the most difficult cases of FIRES in medical history. Our prayers are with you and your family that Drew with continue to quickly recover. Our daughter Jeanette was in the Oklahoma play with Drew.
All the best,
Deric
I was also with Drew on Mr. Taylor’s choir tour last year. Awesome kid.
Wahoo. So relieved he is doing so much better.
Such good news! Still praying for him everyday.
Praise God! Prayers answered! Hugs all around! 💕
I have goose bumps all over. So excited for your families future. Drew is amazing as is your family. I hope you all know how much your blog is helping others. It is giving others hope and strength. I am hoping that by sharing this with a friend I have in Utah it will help bring his son back to the church. He suffers from seizures. This happened after he returned from his mission. He has been angry with God for a while
He still lives a gospel inspired life. He is angry as he still has his seizures and no one knows why.
May God continue to bless Drew and your family. I so look forward to hearing from you every week. I keep you all in my prayers.
God bless
Tanya Baptie
Prayers answered. SO happy to hear about this miracle turn around. I am sure he will continue to get better every time
So many tears of joy! My heart is full of gratitude for prayers answered. My kids have been praying for Drew non-stop, and tonight their testimony of prayer has been strengthened. They realize it’s still in the Lord’s hands, and sometimes the answers aren’t the outcome we hoped for. But they see above all that Drew’s positive outcome is being magnified directly by the Lord and Drew is being uplifted and strengthened by the power of prayers. Thank you for your generosity and graciousness in sharing this so many could be part of your journey of faith.
Wonderful news. Faith fills us with peace and helps us to continue forward. Faith brings gratitude to our hearts and opens our eyes to the miracles.
Hugs to you Dawn and family.
I don’t know Drew but I know and love his grandma Judy Olsen. I pray for him every day and am so happy to read of his progress👍😀😀😇
I’m so happy for your family! Drew and Alex are amazing guys (they worked with me at KOPFC). Drew has been in our family’s prayers daily. Keep up the great work, Drew!